
Iowa governor plans to appeal block on restrictive abortion law
Iowa Gov. Kim Reynolds said on Tuesday that plans are in progress to appeal a temporary block on the state's new, restrictive abortion law, previewing a likely emotional court battle that could take months to resolve. Reynolds told reporters at the Iowa Capitol that her staff is working with lawyers in Attorney General Brenna Bird's office to work out the details, so “it's just a matter of time,” she said. The Republican-controlled Legislature approved the measure to ban most abortions after about six weeks of pregnancy during a special session last week, and it went into effect Friday, immediately after Reynolds signed it. The ACLU of Iowa, Planned Parenthood North Central States and the Emma Goldman Clinic launched a legal challenge and on Monday, Judge Joseph Seidlin granted their request to pause the law as the courts assess its constitutionality. Abortion providers said they scrambled to fit in as many appointments as possible before the governor signed the bill, making hundreds of calls to prepare patients for the uncertainty and keeping clinics open late. After the ruling, providers at Planned Parenthood and the Emma Goldman Clinic indicated they were relieved but conscious of the long legal fight ahead. “I think the bill that we passed is constitutional, especially with the changes that we’ve seen," said Reynolds, who alluded to the Iowa Supreme Court and the U.S. Supreme Court reversing previous rulings that affirmed a woman's fundamental right to abortion. “We passed it, it went into law, and for three days we were saving babies,” she said. “I think the right to life is the most important right that we have.” Read More Ukraine war’s heaviest fight rages in east - follow live Charity boss speaks out over ‘traumatic’ encounter with royal aide
2023-07-19 05:24
What's the Best iPad to Buy in 2023?
iPads dominate the US tablet market for good reason. Apple has a great set of
2023-10-17 21:51

John Woo's 'Silent Night' trailer teases a mute father's bloody revenge after a Christmas tragedy
The official trailer for John Woo's Silent Night has arrived, demonstrating exactly how silent this
2023-10-04 00:53

Workers strike at major Southern California hotels over pay and benefits
Workers are picketing major Southern California hotels after walking off the job during the holiday weekend to demand better pay and benefits
2023-07-04 06:15
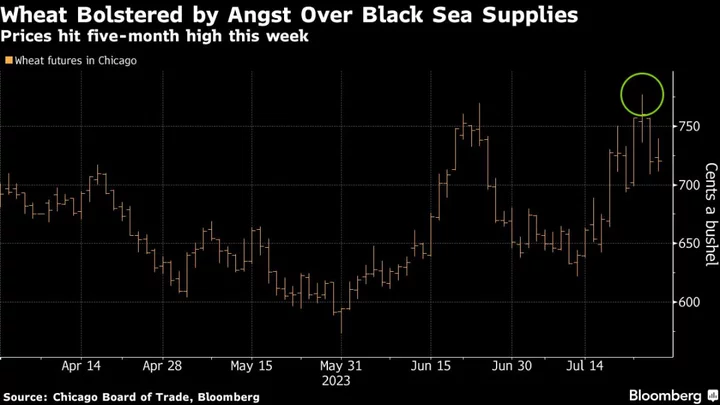
Putin Rewards African Allies With Promise of Free Grain
Russian President Vladimir Putin promised to send free grain to six African countries that have strong ties with
2023-07-27 21:29

New York Times Columnist David Brooks' $78 Airport Meal Is Remarkable
New York Times columnist David Brooks' $78 airport meal is fantastic.
2023-09-21 21:24

Nothing Phone (2) Launching in the US Without Carrier Constraints
It looks like the Nothing Phone (2) will launch in the US in July as
2023-05-26 03:48

‘Long Covid has taken away my ability to eat food or urinate - I don’t recognise myself anymore’
A young woman whose health “deteriorated rapidly” after being diagnosed with long Covid and suffering a liver bleed is now in a wheelchair, feeds herself through a tube in her chest and has been unable to urinate in three years. Abigail Snowball, 29, was told she suffered from a rare condition known as Fowler’s Syndrome a few months after she was diagnosed with long Covid in July 2020 and her bladder stopped working. The social worker, from Northumberland, says she was “never sick” and enjoyed long runs before testing positive for coronavirus in early 2020 and feeling a sharp pain under her ribs which scans showed was a bleed on her liver. Abigail had not fully recovered from the virus and since the diagnosis, her health has gone from bad to worse, to the point where she has not been able to urinate in three years. She now depends on her husband Mark, 34, to carry her to the bathroom so she can empty her bladder, which can take up to four hours, and has not been able to enjoy a mouthful of food for nearly a year. “I had never really been ill before,” Abigail told PA Real Life. “As a child, I was always really lucky and never poorly. I look back at pictures from before Covid and I don’t even recognise myself.” Abigail had completed a 20-mile race, the Run Northumberland BIG 20, just a week before testing positive for Covid and having to quarantine away from Mark, who works in maintenance for Nissan. “It was very much at the start of the pandemic, back at the time when there weren’t any vaccines or much testing,” she said. “It was just tiredness like I’ve never felt before in my entire life. I remember having a cup of tea and struggling to lift the mug up.” Like many other people’s experience of catching Covid, Abigail’s health improved over the next 10 days. “I did get better, but I never fully recovered,” she said. But a couple of months later, while visiting her parents, Jane and Ray Cresswell, in Cornwall on holiday, she suddenly began feeling a sharp pain under her ribs. “It was a really strange location to have pain,” she added. She visited the GP a week later and was admitted to Northumbria Specialist Emergency Care Hospital (NSECH) in July 2020, where scans revealed Abigail had suffered a bleed on her liver. “That’s when they diagnosed me with long Covid,” she said. “There was no other explanation, because they tested for blood disorders and carried out a scan. “They asked me if I had a fall or accident, but there was literally nothing.” Abigail was recovering from her liver bleed in hospital late one evening when a nurse asked when the last time she urinated was. “I actually thought, ‘god, it wasn’t since this morning’,” she said. “From that point, my bladder never regained any function. That was really the start of my health declining quickly.” Doctors hoped her bladder block was simply a result of the liver “trauma” and that she would be on the mend soon. But, sadly, this was not the case. A few months later, Abigail was diagnosed with a rare condition called Fowler’s Syndrome, which causes women to have problems passing urine. Abigail’s condition has deteriorated over the past few weeks and she is now losing weight rapidly. “I am now sleeping on the sofa downstairs and my husband Mark is having to carry me to the toilet and back again,” she said. “We can spend up to four hours at a time trying to drain my bladder, and the pain is just unbearable. “I went from running 20 miles to using a wheelchair. You don’t realise how inaccessible the world is until you are in that position.” Since the diagnosis, Abigail has spent more than 350 days in hospital and undergone 12 surgeries, including one in October 2021 to try and reconstruct her bladder. To make matters worse, she developed intestinal failure last year, which means she can no longer eat food. “I haven’t eaten anything in a year now,” she said. Instead, she is fed through TPN (total parenteral nutrition), a tube in her chest which delivers nutrients directly into the blood stream. Abigail and Mark, who married earlier this year in May, both received close to six months of training on how to perform the feeding procedure given there is a high risk of infection. “We had never even heard of that – being fed through a line into your heart,” she said. Abigail has been told by doctors that her liver bleed was “extremely likely” to have been caused by Covid. While Covid is known to harm the lungs, it has also been found to affect other organs, including the heart, liver and kidneys, but wider research is needed to better understand its long-term effects. Liver problems are common among patients with Covid-19, according to a study carried out by researchers at Oxford University and published in the peer-reviewed journal Hepatology Communications. Abigail, whose condition is considered “severe”, is hoping to receive specialist treatment in London, known as bladder Botox, which involves injecting Botox into the bladder every three to nine months, but there is no guarantee this will work. “Because of how severe and complex my case is, we’ve exhausted all our options here and the doctors are saying that I need to see the specialists in London,” she said. “Removing my bladder completely remains on the cards, but it’s incredibly high risk because of my intestinal problems. “There is no cure for Fowler’s, so it’s about managing it in the best way possible.” The combination of health conditions has left Abigail unable to perform everyday tasks. “It’s funny because the things I want to be able to do are so normal,” she said. “Just being able to wake up, take the dog for a walk and go to work. “Things that in the past, I completely took for granted.” To help cover the costs, Abigail’s friend Emma Holt has set up a GoFundMe which has received thousands of pounds in donations. “We never imagined in our wildest dreams that we would raise the amount of money that we have already,” she said. “It’s the one thing that really keeps us going, when things are really difficult. “Knowing that we have so many people behind us and supporting us is amazing.” Fowler’s Syndrome is most often caused by infection or following surgery or trauma, but a link to long Covid has yet to be established and more research is needed. Dani Coombe, CEO, Fowler’s Syndrome UK said: “It’s too early to say if long Covid is a trigger for Fowler’s syndrome; we haven’t seen an increase in Fowler’s and retention post-Covid yet, and there is no indicator that urinary retention gets worse. “Our research into what patients believe triggered their urinary retention shows that infection is the most common trigger at 57 per cent, followed by surgery in 32 per cent of patients and trauma at 19 per cent. “It would be noteworthy to see in coming years if there is an increase in women with Fowler’s because of the trauma of Covid-19.” Read More Fake meat is dying, but that shouldn’t mean the end of veganism What I gained (and lost) from walking 10,000 steps a day for five months Woman behind ‘not real’ plane tirade identified as marketing executive with $2m home Charity boss speaks out over ‘traumatic’ encounter with royal aide Ukraine war’s heaviest fight rages in east - follow live
2023-08-10 18:52

Isn’t It Ironic? Way Day’s Best Bedding Deals Have Us Wide Awake
When we're not scavenging for loveseats or scouting out cushy office chairs over at the massive online home goods hub Wayfair, we're strolling through its virtual bedding aisle. Especially when the retailer's infamous 48-hour sale event Way Day has duvet cover sets, cooling pillows, mattress toppers, and more bedding essentials up to 70% off.
2023-10-27 04:26

Is it heat exhaustion or are you just tired?
Whether you’re away on holiday or lounging in the sun at home, needing a siesta after lunch or a disco nap before dinner on a hot summer’s day is normal. But how can you tell when warm weather-induced drowsiness is something more serious? We asked doctors to explain… What is heat exhaustion? “Prolonged exposure to the heat can cause heat exhaustion. It is the body’s response to excessive loss of water and salt,” says Dr Preethi Daniel, deputy medical director at London Doctors Clinic. “Symptoms may be characterised by heavy sweating, rapid breathing, headache, high temperature, nausea, a faster and weak pulse, light-headedness, feeling fatigued and heat cramps.” Older people, babies, children and those with chronic illnesses are much more likely to develop heat exhaustion. “Symptoms are usually the same in adults and children, and can make children tired and floppy,” says Dr Luke Powles, associate clinical director at Bupa Health Clinics. While not life-threatening, heat exhaustion is a warning sign that you need to cool down promptly to prevent progression to heat stroke, which means getting out of the sun immediately. “Remove any unnecessary clothing, lie down and raise your feet so they are above the level of your heart and drink plenty of water,” says Powles. “You can also use a cool sponge to cool your skin. Make sure someone stays with you until you feel a bit better – which you should do in half an hour or so.” If you don’t start to cool down after 30 minutes, see medical help, as you may have developed heatstroke. What is the difference between heat exhaustion and tiredness? “Heat exhaustion is the direct result of spending too much time in the sun and often raises your core body temperature to over 38 degrees, which isn’t an indicator of general tiredness,” says Dr Carolyn Barshall, GP at independent charitable hospital King Edward VII’s. “Whereas tiredness can be caused by many lifestyle factors such as disordered sleeping patterns, alcohol and poor diet.” Daniel adds: “If you have a lack of energy or aches and pains, consider it tiredness, but if you have any of the other symptoms mentioned above, it could be heat exhaustion.” What is heatstroke? “Heatstroke is the end result of overheating,” says Daniel. “Our internal temperature rises and creates confusion, drowsiness and can lead to seizures.” Much more serious than heat exhaustion, it can cause a change in mental status such as, Barshall says: “Confusion, delirium, combativeness, seizures, loss of consciousness, and a core body temperature above 40 degrees.” Symptoms may also include skin that’s not sweating even when it feels hot, fast breathing or shortness of breath. “Heat exhaustion and heatstroke are often confused, but there is a difference,” says Powles. “Heatstroke should be treated as an emergency, whereas with heat exhaustion, the person needs to be cooled down.” If you suspect someone has heatstroke you should call 999 or seek emergency help immediately. How to stay safe in the sun To prevent heat exhaustion during summer, it’s important not to spend too long in the sun and to stay hydrated. “Avoid direct sunlight between 11am and 3pm, and wear light-coloured, loose clothing,” says Daniel. “Drink plenty of cold drinks and water throughout the day and limit alcohol intake.” To help little ones, she says: “You can keep a pram or buggy cool by covering it with a damp cloth and refreshing it every 30 minutes.” Read More Charity boss speaks out over ‘traumatic’ encounter with royal aide Ukraine war’s heaviest fight rages in east - follow live King Charles enjoys a wee dram at the Met Highland Gamesv Why have the birds disappeared from my garden? Top Films: w/c Saturday, August 12
2023-08-07 14:45

The best automatic cat feeders for your furry friend
If you plan on being away for a couple days or you've started your cat
2023-08-30 19:45

Brain’s appetite control centre different in overweight or obese people – study
The brain’s appetite control centre is different in the brains of people who are overweight or live with obesity, a new study suggests. The researchers said their findings add further evidence to the relevance of brain structure to weight and food consumption. Current estimates suggest that more than 1.9 billion people worldwide are either overweight or obese. And, according to the Office for Health Improvement and Disparities, almost two-thirds of adults in the UK are overweight or living with obesity. This increases the risk of developing health issues like type 2 diabetes, heart disease and stroke, cancer and poorer mental health. The last two decades have given us important insights about appetite control and how it may be altered in obesity Professor Paul Fletcher, University of Cambridge A number of factors influence how much people eat and what they eat, including genetics, hormone regulation, and the environment they live in, researchers say. However, it is not entirely clear what happens to the brain to tell us that we are hungry or full. Past studies have shown that the hypothalamus – a small region of the brain about the size of an almond – plays an important role. Dr Stephanie Brown, from the Department of Psychiatry and Lucy Cavendish College, University of Cambridge, said: “Although we know the hypothalamus is important for determining how much we eat, we actually have very little direct information about this brain region in living humans. “That’s because it is very small and hard to make out on traditional MRI brain scans.” Professor Paul Fletcher, the study’s senior author, from the Department of Psychiatry and Clare College, Cambridge, said: “The last two decades have given us important insights about appetite control and how it may be altered in obesity. “Metabolic researchers at Cambridge have played a leading role in this. “Our hope is that, by taking this new approach to analysing brain scans in large datasets, we can further extend this work into humans, ultimately relating these subtle structural brain findings to changes in appetite and eating and generating a more comprehensive understanding of obesity.” The majority of evidence for the role of the hypothalamus in appetite regulation comes from animal studies, which indicate complex interacting pathways within the hypothalamus, with different cell populations acting together to tell us when we are hungry or full. To get around this researchers used an algorithm developed using machine learning to analyse brain scans taken from 1,351 young adults across a range of BMI scores. They looked for differences in the hypothalamus when comparing individuals who are underweight, healthy weight, overweight, or living with obesity. According to the findings, the overall volume of the hypothalamus was significantly larger in the overweight and obese groups of young adults. The researchers describe a significant relationship between volume of the hypothalamus and body mass index (BMI). The differences were most apparent in those sub-regions of the hypothalamus that control appetite through the release of hormones to balance hunger and fullness. While the exact significance of the finding is unclear, one explanation is that the change relates to inflammation, the researchers suggest. Eating a high-fat diet could trigger inflammation of our appetite control centre Dr Stephanie Brown, University of Cambridge Previous animal studies have shown that a high-fat diet can cause inflammation of the hypothalamus, which in turn prompts insulin resistance and obesity. In mice, just three days of a fat-rich diet is enough to cause this inflammation. Other studies have shown that this inflammation can raise the threshold at which animals are full – in other words, they have to eat more food than usual to feel full. Dr Brown added: “If what we see in mice is the case in people, then eating a high-fat diet could trigger inflammation of our appetite control centre. “Over time, this would change our ability to tell when we’ve eaten enough and to how our body processes blood sugar, leading us to put on weight.” More research is needed to confirm whether increased volume in the hypothalamus is a result of being overweight or whether people with larger hypothalami are predisposed to eat more in the first place. It is also possible that these two factors interact with each other, causing a feedback loop, the study published in Neuroimage: Clinical, and supported by the Bernard Wolfe Health Neuroscience Fund, Wellcome and the NIHR Cambridge Biomedical Research Centre, with additional funding from Alzheimer’s Research UK, suggests.
2023-08-08 16:15
You Might Like...

Alipay+ Partners With PayNet to Promote Seamless Payment for Inbound and Outbound Malaysian Travellers

Build Healthy Habits With MyFitnessPal

Christian Cowan launches limited edition Candy Crush beanbag dress
You'll be able to book flights through Uber soon

Feel Like Puking? Mark Zuckerberg Shows Off VR/AR Tech Inside a Moving Car

Slovakia campaign rhetoric raises LGBTQ concern

Turkish Airlines Mega Plane Order Taking More Time to Wrap Up

The best travel app is an iPhone feature you're probably ignoring
